Tick-borne infectious diseases
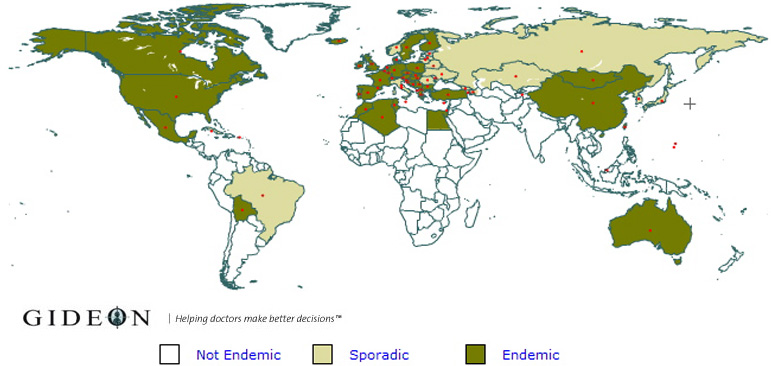
Tick-borne infectious diseases
Tick- and flea-borne infectious diseases in dogs and cats (backgrounder)
Cats and dogs have always been subject to tick and flea infestations; however in recent years the diseases transmitted by these parasites (known as vector-borne diseases) have become more widespread, posing a very real threat to both pets and humans.
These changes have come about as a result of a complex interplay between many factors, including: increased rates of pet ownership
increasing numbers of pets kept inside the house and allowed access to human sleeping areas, etc.
increased frequency and duration of pet travel leading to the movement of infected ticks to new geographic areas
increasing travel to countries with endemic vector-borne diseases
changes in urban planning that increase ‘tick-friendly’ green spaces in urban areas
wildlife protection efforts that increase numbers of alternative hosts for ticks, such as foxes
climatic changes that allow diseases previously restricted to warmer climates to spread north, and less severe winters that result in fewer tick deaths.
Many people may be already aware that flea infestations in pets can occur all year round, however it is less well-known that climatic changes have also led to tick infestations occurring more frequently outside of traditional peak seasons. With the risk of infestation and related diseases remaining throughout the year, a number of expert groups recommend that pet flea and tick preventative treatment should be maintained year round.
The most effective approach to dealing with tick- and flea-borne diseases is to prevent transmission. This can be achieved by repelling the parasite vectors that transmit these potentially lethal diseases. The use of parasiticides with repellent activity has been demonstrated to reduce the risk of potentially lethal vector-transmitted diseases under laboratory as well as field conditions.
Tick-borne infectious diseases
There are around 800 species of tick worldwide, broadly categorised as either ‘hard’ (or ixodids) or ‘soft’ (or argasids). Soft ticks feed quickly and are rarely a cause of disease burden. The approximately 400 species of hard ticks remain attached to a host for as much as several days, and pose a threat to pets and humans as they can potentially transmit infection between hosts, and even between species.
The main hard tick species affecting pets in Europe are Ixodes ricinus (the sheep tick, deer tick or castor bean tick), Dermacentor reticulatus (marsh tick or ornate cow tick) and Rhipicephalus sanguineus (Brown Dog Tick). Together, these ticks are responsible for the transmission of a number of serious diseases in companion animals, including:
Anaplasmosis: can cause acute fever and significantly damage the immune system of dogs and cats. Anaplasmosis appears to be a largely self-limiting infection in dogs.
Babesiosis: causes fever with severe, progressive haemolytic anaemia in dogs. Diagnosed only sporadically in cats where disease tends to be chronic and low-grade until stressed. Infection causes long-term damage to kidneys, liver and Central Nervous System (CNS).
Ehrlichiosis: causes fever, weight loss, eye and nose discharge, as well as thrombocytopenia and anaemia in dogs, but is rarely diagnosed in cats. Long-term subclinical infection is common in dogs; however, severe life-threatening chronic ehrlichiosis can arise following persistent infection. Ehrlichiosis is more severe in certain breeds (e.g. German Shepherd) and in younger animals.
Lyme borreliosis: affects cats and dogs as well as humans. Although a high proportion of dogs are seropositive in endemic areas, relatively few develop clinical signs such as lameness, fever, loss of appetite and fatigue. Persistent infection with Borrelia spp. even after antibiotic therapy is reportedly common in dogs.
Mediterranean Spotted Fever (MSF)/boutonneuse fever: MSF can be found in dogs and humans in Southern Europe, the Middle East and Southern Africa, but clinical signs have not been reported in dogs. In humans, symptoms include high fever, severe headache, rash and photophobia.
Tick-borne encephalitis (TBE): caused by a Flavivirus, TBE is found across northern and eastern Europe where it is spread by I. ricinus. Traditionally appearing in two peaks in late spring and early autumn periods, climatic changes are extending the risk period for TBE. Three subtypes of TBE exist, with the more easterly forms associated with greater morbidity and mortality in humans. While TBE can manifest in dogs, it is a less severe disease, with low risk of developing clinical symptoms including paralysis. In humans, clinical symptoms appear in 30% of infected individuals. The majority of symptomatic patients experience flu-like symptoms, however 10-15% will develop neurological effects including meningoencephalitis, and paralysis. Death rates vary depending on subtype, from 1-5% in Central Europe to 25-30% in the Far Eastern (or Russian Spring/Summer) form.
Several of the tick-borne infections that affect companion animals can cause serious diseases in humans, notably Lyme borreliosis, anaplasmosis, RMSF, Mediterranean Spotted Fever and tick-borne encephalitis.
Infection with multiple tick-transmitted pathogens, or with multiple genotypes of the same pathogenic species, can occur in an individual animal following heavy exposure to ticks. The same tick species can be a vector for several pathogens, and coinfection of individual ticks can occur. In dogs, coinfection with combinations of Ehrlichia, Bartonella, Babesia, Hepatozoon, Leishmania and Rickettsia species occur in endemic areas.
Flea-borne infectious diseases
Like ticks, fleas are capable of spreading a number of diseases that affect cats, dogs and humans. Fleas are also being aided by the changes in climate, leading to longer seasons and fewer fleas being killed off over winter, and by changes in pet ownership. The increasing use of central heating in colder climates and the greater physical closeness between pets and owners in particular have helped fleas to remain the most common ectoparasite in cats and dogs.
While there are a number of species of flea, the most important species in European pets are Ctenocephalides felis (the cat flea), Ctenocephalides canis (the dog flea) and Pulex irritans (the human flea). While each has its preferred hosts (as indicated by their common names), they are also capable of infesting other species.
Diseases caused or spread via fleas include:
Dog tapeworm (Dipylidium caninum): despite the name, the Dipylidium caninum tapeworm can infect cats and humans, particularly children, as well as dogs. Symptoms may include mild weight loss along with itching around the anal area caused by passing segments of tapeworm.
Flea allergy dermatitis (FAD): one of the most frequent causes of skin conditions in small animals and a major clinical issue in dogs and cats. Symptoms include rashes and swelling along with self-trauma due to excessive scratching. Prolonged exposure can lead to chronic lesions, alopecia, infection and changes to skin structure.
Bartonellosis: a number of Bartonella species are now known to be zoonotic and use pets as reservoirs. The most well known of the bartonella spp is Bartonella hensellae, which causes the disease commonly known as ‘cat scratch disease‘. As with other Bartonella species, B. hensellae can be transmitted either via the feeding of fleas or directly by biting or scratching. Clinical manifestation of Bartonella infection can range from asymptomatic infection, to severe disease and sudden death. Clinical signs related to Bartonella infection in dogs include: endocarditis, myocarditis, anaemia, hepatitis, polyarthritis, uveitis, choroiditis, weight loss and epistaxis. Cats do not appear to usually develop symptoms as a result of Bartonella infection.
Flea-borne spotted fever (caused by Rickettsia felis): only emerged as a disease in humans in the 1990s, flea-borne spotted fever has since been discovered to be widely present in cat fleas around the world. Infection in humans leads to fever, rash, headache, abdominal pain, hearing loss and meningitis, while infection in dogs appears to produce fatigue, diarrhoea and vomiting without fever. Cats, however, have not been shown to demonstrate any symptoms.
Murine or endemic typhus (caused by Rickettsia typhi): although usually transmitted through the rat flea, Rickettsia typhi can also be transmitted via the cat flea. While rare, symptoms are similar to Rocky Mountain Spotted Fever (RMSF).
Plague (caused by Yersinia pestis): Although believed to be a rare occurrence, the cat flea has been found to be capable of transmission of bubonic plague. Cats infected with Yersinia pestis usually present with bubonic plague, experiencing an extremely high fever, anorexia and swollen lymph glands and have high mortality rates. Dogs appear to be much less likely to develop clinical symptoms.